A guide to physical therapy from the American Physical Therapy Association
What is plantar fasciitis?
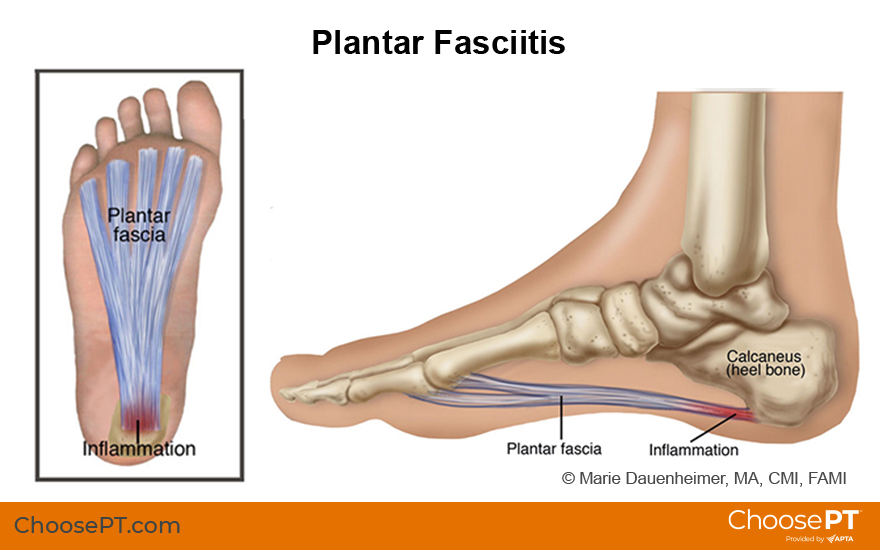
Plantar fasciitis is a foot condition that develops when repeated activities put a strain on the plantar fascia, a thick band of tissue that supports the arch of the foot. People diagnosed with plantar fasciitis also may have heel spurs, a bony growth that forms on the heel bone.
Plantar fasciitis occurs most frequently in people in their 40s, but can occur in all age groups.
The condition can develop in athletes who run or jump a great deal, and in people who have jobs that require them to be on their feet for most of the day, such as police officers, cashiers, or restaurant workers.
Signs and symptoms
Symptoms of plantar fasciitis often appear with a sudden increase in activity. You might feel a stabbing pain on the underside of your heel and a sensation of tightness and/or tenderness along your arch.
People with plantar fasciitis may experience pain:
- In the morning, when stepping out of bed and taking the first steps of the day.
- When standing for a long time.
- When standing up after sitting for a long time.
- After intense activity such as running or jumping.
- When climbing stairs.
- When walking barefoot or in shoes with poor support.
Your pain can fluctuate during the day, with pain improving as your body warms up and worsening later in the day after activity. As the condition gets worse, you may begin to limp.
How is it diagnosed?
The physical therapist’s diagnosis is based on your health and activity history and on a clinical evaluation. Your physical therapist also will take a medical history to make sure that you do not have other conditions that may be causing your pain. Sharing information about your work and recreation and reporting any lifestyle changes will help your physical therapist diagnose your condition and tailor a treatment program for your specific needs.
To diagnose plantar fasciitis, your physical therapist may conduct the following physical tests to see if symptoms occur:
- Massaging and pressing (palpation) on the heel area, arch of the foot, toward the toes.
- Gently stretching the ankle to bend the top of the foot toward the leg (dorsiflexion).
- Gently pressing the toes toward the ankle.
How can a physical therapist help?
Physical therapists are trained to evaluate and treat plantar fasciitis. When you are diagnosed, your physical therapist will work with you to develop a program to decrease your symptoms. Your treatment may include:
- Assessment of your gait (how you walk) and how this may impact your symptoms.
- Stretching exercises to improve the flexibility of your ankle and the plantar fascia.
- Strengthening exercises to improve the strength of supporting muscles.
- Application of ice to decrease pain and inflammation.
- Iontophoresis (a gentle way to deliver medication through the skin).
- Taping of the foot for short-term relief.
- Orthotics (shoe inserts) and supportive footwear to minimize abnormal foot motion or to help support your arch, reducing stress to the plantar fascia.
- A night splint to help you maintain correct ankle and toe positions while sleeping.
- Gait training to help lessen symptoms and improve your walking ability.
Research shows that most cases of plantar fasciitis improve over time with these conservative treatments, and surgery is rarely needed.
Can this injury or condition be prevented?
Factors that contribute to the development of plantar fasciitis include:
- Age (over 40 years)
- A job, sport, or hobby that involves prolonged standing or other weight-bearing activity
- Rapid increases in length or levels of activity, such as beginning a new running program or changing to a job that requires a lot of standing or walking
- Decreased calf muscle flexibility
- Increased body weight (Body Mass Index greater than 30)
- Flat feet
- Wearing shoes such as high heels, or those with inadequate arch support
Guidelines for the prevention or management of plantar fasciitis include:
- Choosing shoes with proper arch support and heel height.
- Replacing your shoes regularly before they wear out.
- Using a thick mat if you must stand in one place for much of the day.
- Adjusting your exercise program to include a warmup and a gradual buildup to avoid straining the plantar fascia.
- Stretching your calves and feet before and after running or walking.
- Maintaining a healthy body weight.
Your Welia Health physical therapist will design an individualized treatment program to help heal your plantar fasciitis and prevent future injury. Physical therapy services are available in Mora, Hinckley and Pine City. To learn more or schedule an appointment, call Rehabilitation Services at 320.225.3356.
References
- McClinton SM, Heiderscheit BC, McPoil TG, Flynn TW. Effectiveness of physical therapy treatment in addition to usual podiatry management of plantar heel pain: a randomized clinical trial. BMC Musculoskelet Disord, 2019;20(1):630.
- Grim C, Kramer R, Engelhardt M, et al. Effectiveness of manual therapy, customised foot orthoses and combined therapy in the management of plantar fasciitis—a RCT. Sports (Basel). 2019;7(6):128.
- Thong-on S, Bovonsuthonchai S, Vachalathiti R, et al. Effects of strengthening and stretching exercises on the temporospatial gait parameters in patients with plantar fasciitis: a randomized controlled trial. Ann Rehabil Med. 2019;43(6):662–676.
- Lee JH, Park JH, Jang WY. The effects of hip strengthening exercises in a patient with plantar fasciitis: a case report. Medicine (Baltimore). 2019;98(26):e16258.
- Arnold MJ, Moody AL. Common running injuries: evaluation and management. Am Fam Physician. 2018;97(8):510–516.
- Kirkpatrick J, Yassaie O, Mirjalili SA. The plantar calcaneal spur: a review of anatomy, histology, etiology and key associations. J Anat. 2017;230(6):743–751.
- Lim AT, How CH, Tan B. Management of plantar fasciitis in the outpatient setting. Singapore Med J. 2016;57(4):168–171.
- Landorf KB. Plantar heel pain and plantar fasciitis. BMJ Clin Evid, 2015;2015:1111.














