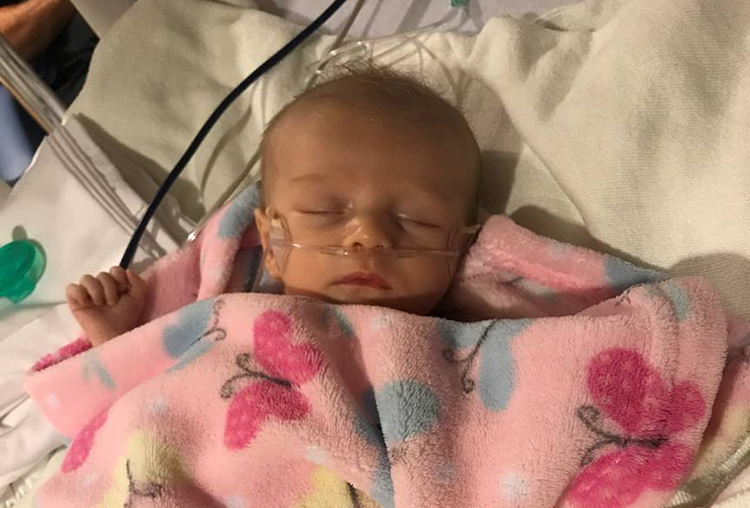
Mom with Type 1 diabetes delivers healthy baby girl
Pregnant with her third child, Carly Gahler, RN, BSN, a diabetes educator at Welia Health, saw the pandemic preparation unfold in her weekly prenatal appointments.
One week, clinic staff were wearing face masks. The next week they were donning face shields. And the next, scrubs and gowns. Guidelines for personal protective equipment (PPE) were changing as rapidly as new information about the virus arose and availability shifted. Carly had been working from home, so her prenatal appointments gave her a window into Welia Health’s COVID-19 response as a patient.
“I have Type 1 diabetes, which requires a little extra care for mom and baby. Starting at 32 weeks, which for me was early on in March, I was in the clinic twice a week for various appointments, just as everything was starting with COVID. Even though everyone was in masks, and you could only see their eyes, I could feel the warmth and love from the Welia Health team.”
Carly Gahler, Welia Health Diabetes Educator and recent Birthing Center Patient
Diabetes and pregnancy
Although Welia Health was increasing the use of virtual visits, Carly had to physically go to the clinic for her appointments. When pregnant women have Type 1 diabetes, they must complete a weekly biophysical profile starting at 32 weeks. This assessment checks four main categories of the baby’s health – heart rate, fluid level, tone and movement.
While there is a list of complications that can arise with diabetes in pregnancy, the two main concerns are hypoglycemia, a condition where blood sugar can drop to be dangerously low, and larger than average birth weight. Another concern for expectant mothers with diabetes is that continued high blood sugars can cause an increase in amniotic fluid, much more than they need. So, every four weeks, providers recommend a growth ultrasound to make sure the baby doesn’t grow too large or too rapidly. Throughout the pregnancy, both Carly’s and her baby’s assessments came back fine.
A new way of working
In her role as a diabetes educator, Carly focuses on these biophysical assessments when working with expectant mothers with Type 1, 2 and gestational diabetes. She closely monitors her patients, doing everything possible to keep moms and babies safe.
Due to the COVID-19 pandemic, any high-risk employees were asked to work from home to reduce their exposure. “I worked up until the Friday before the Monday I had my baby. The ability to work from home when you’re pregnant is wonderful – you don’t have to worry about which clothes fit at nine months,” Carly chuckled. “I was fortunate that most of my job duties were able to be done from a home office.”
Scheduled C-section
Carly’s first two pregnancies resulted in emergency c-sections, so with a scheduled c-section she liked having the chance to prepare a little more for her baby’s birth. Plus, the Governor’s Stay-at-Home orders during the pandemic allowed her plenty of time to make sure all the preparations were made. She even made sure her husband Traver’s bag was packed because new hospital rules did not allow him to leave and reenter.
Delivery among friends

“A planned c-section was a completely different – and much improved – delivery experience than with my previous emergency c-sections,” commented Carly.
Dr. Matthew Schultz delivered Carly’s healthy baby girl, Madelyn, on June 15 at 8:05 am. She weighed 8 pounds and 9 ounces.
“Having my baby at Welia Health was just a wonderful experience,” said Carly. “Given COVID, we couldn’t have visitors, but knowing all of the staff, many quickly stopped by to say hello and wish us well. I could literally feel the compassion from the nurses because they just take such great care of their patients.”
Madelyn was born in the new birthing center. Carly remarked that the rooms are beautiful with large windows allowing in a ton of natural light. She loved having her husband and baby in the room with her.
“Other than a few hints of change and encouraged masking, there wasn’t anything major that made delivering during a pandemic too different,” said Carly. “The whole process was quite comforting. In fact, not having visitors was nice in a way because Traver and I had that time to focus on my recovery and just bond with Madelyn.”
Adjusting to a zone defense
Madelyn has two big adoring brothers, Mason who is six, and Milo who is three. When Carly, Traver and Madelyn were in the hospital, they FaceTimed with the boys, yet only talked for a bit because they were off running and playing. But now that everyone is home and adjusting, it is much different.
“Mason and Milo are just enamored with Madelyn and love her to pieces,” said Carly. “Milo is normally our wild one, always wrestling with his big brother. But now has been so gentle with his little sister, holding her and even singing to her. It’s like a switch flipped in him and he has become a protector and caregiver. Mason is just excited to be a big brother again.”
Carly also has enjoyed seeing Traver be a father to a daughter. Her husband loves to wrestle with the boys, but she is finding his tone with Madelyn so sweet. Carly feels a different vibe when she watches Traver cuddling with his daughter or when he’s simply holding her. She’s enjoying the nuance.
The new parents of three are a little intimidated by being outnumbered. With family close by, Carly is thankful for the help and support she can count on. Having three kids will be a big change, but it’s one Carly and Traver are ready for, particularly as they watch their boys with their baby sister.
Most details of a birthing experience are forgotten in a few years, but Carly will remember this experience as one in a lifetime – giving birth during a pandemic, now being outnumbered, and adjusting to a whole new normal.